Seeking Health Insurance Policy? Get big relief from confusing products soon
IRDAI Standard Health Product Guidelines: In what may provide a big relief to Health Insurance seekers, the Insurance Regulatory and Development Authority of India (IRDAI) has issued new guidelines

IRDAI Standard Health Product Guidelines: In what may provide a big relief to Health Insurance seekers, the Insurance Regulatory and Development Authority of India (IRDAI) has issued new guidelines for standard health product by all insurers including general and health insurance businesses. When implemented, the IRDAI guidelines will stop the practice of selling health insurance schemes with different offers. Companies will have to provide similar cover in similar health insurance products. The guidelines say the minimum basic sum insured under standard product shall be Rs 50,000 and the maximum limit shall be Rs 10 lakh.
After the implementation of the new guidelines, companies would not be able to offer add-on or optional products along with the general health insurance scheme.
Check Important proposals in the Draft guidelines (Source: IRDAI)
Standard Health Product shall offer only the following "mandatory" covers:
1. Hospitalization Expenses The Hospitalization expenses should cover -
a) Room, Boarding, Nursing Expenses all inclusive as provided by the Hospital/Nursing Home
b) Surgeon, Anaesthetist, Medical Practitioner, Consultants, Specialist Fees whether paid directly to the treating doctor/surgeon or to the hospital
c) Anaesthesia, blood, oxygen, operation theatre charges, surgical appliances, medicines and drugs, costs towards diagnostics, diagnostic imaging modalities, and such other similar expenses.
- (Expenses on Hospitalization for a minimum period of 24 hours only are admissible. However, this time limit will of 24 hours shall not apply when the treatment does not require hospitalization as specified in the terms and conditions of policy contract, where the treatment is taken in the Hospital and the Insured is discharged on the same day.)
d) Intensive Care Unit (ICU)/Intensive Cardiac Care Unit (ICCU) expenses
e) Expenses incurred on treatment of Cataract subject to sub limits, if any, based on sum insured
f) Dental treatment, necessitated due to an injury
g) Plastic surgery, necessitated due to disease or injury
h) Domiciliary Hospitalization
2. AYUSH Treatment: Expenses incurred on treatment under Ayurveda, Unani, Sidha and Homeopathy systems of medicines shall be covered subject to fixed and standard sub-limits based on Sum Insured.
3. Pre-Hospitalization medical expenses incurred for a period not less than 30 days prior to the date of hospitalization shall be admissible.
Post Hospitalization medical expenses incurred for a period of not less than 60 days from the date of discharge from the hospital towards Consultant fees, Diagnostic charges, Medicines and Drugs wherever required and recommended by the Hospital / Medical Practitioner, where the treatment was taken, following an admissible claim shall be included.
4. Wellness Incentives: To promote and maintain wellness regime, it is considered essential that a wellness and preventive program that incentivises the targeted market segment to start living healthier shall also be incorporated. Accordingly, to enable the individuals to lead longer, healthier and more productive lives, the following wellness features shall be made available to all the insured persons by duly complying with the provisions of Regulation 19 of IRDAI (Health Insurance) Regulations, 2016 and the applicable guidelines notified thereunder.
- Health Check-ups and Consultation services: Under this cover, the insured person shall be made available an access to the health consultations across the network providers or other empanelled hospitals of the insurer, for getting periodic consultation of at least once in a policy year.
- Disease Management: Under this cover, every insured person shall be provided an access to the professional medical services for bettering the health profile. As part of post-hospitalization services follow up care shall be made available, as part of Disease Management. Insurers may also provide other suitable services under this programme.
- Fitness Activities: Under this cover, insurers shall provide parametric indices based on fitness regime being followed by insured person, during the policy tenure and reward mechanism shall be designed so as to incentivize the policyholders to continue with the fitness regime.
- Outpatient consultations or treatments: Under this programme, insured person shall be provided services of outpatient consultations or treatments periodically or based on the pre-determined triggers contingent upon the health of the insured.
Applicable norms:
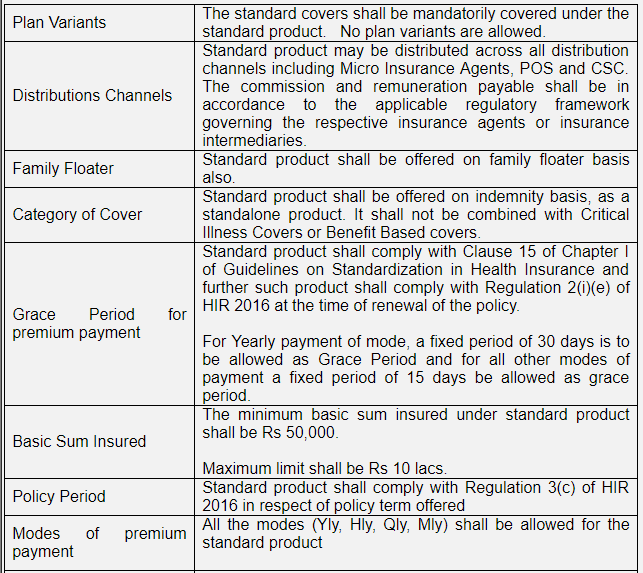
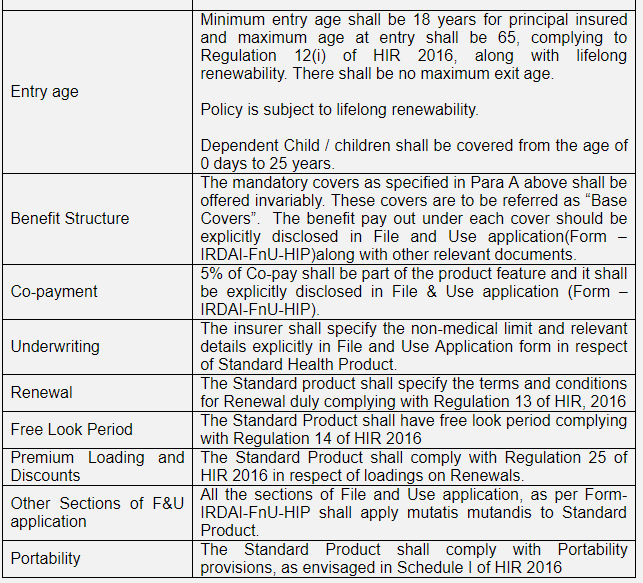
*Source: IRDAI
5. Cumulative Bonus(CB): Sum insured (excluding CB) shall be increased by 5% in respect of each claim free policy period (where no claims are reported), provided the policy is continuously renewed without a break subject to maximum of 50% of the sum insured (excluding CB accrued) under the current policy period.
6. No deductible features are permitted under the base cover.
7. Product name: The nomenclature of the product shall be Standard Mediclaim Policy, succeeded by name of insurance company, (Standard Mediclaim Policy, ). No other name is allowed in any of the documents.
05:47 PM IST





 Insurance regulator IRDAI abolishes age restriction on health insurance
Insurance regulator IRDAI abolishes age restriction on health insurance Irdai introduces changes to life insurance policy surrender value; know what you will get now
Irdai introduces changes to life insurance policy surrender value; know what you will get now  Pay As You Drive (PAYD): Motor insurance ad-on that customises your premium as per driving distance
Pay As You Drive (PAYD): Motor insurance ad-on that customises your premium as per driving distance IRDAI proposes to increase free look period to 30 days for policyholders
IRDAI proposes to increase free look period to 30 days for policyholders Max Financial Services soars after IRDAI approves Axis Bank-Max Life capital infusion deal
Max Financial Services soars after IRDAI approves Axis Bank-Max Life capital infusion deal